- Phone: +919646764444
- Mon-Sat (9am - 2pm & 4pm - 7pm)
- arogyampilesclinic@gmail.com
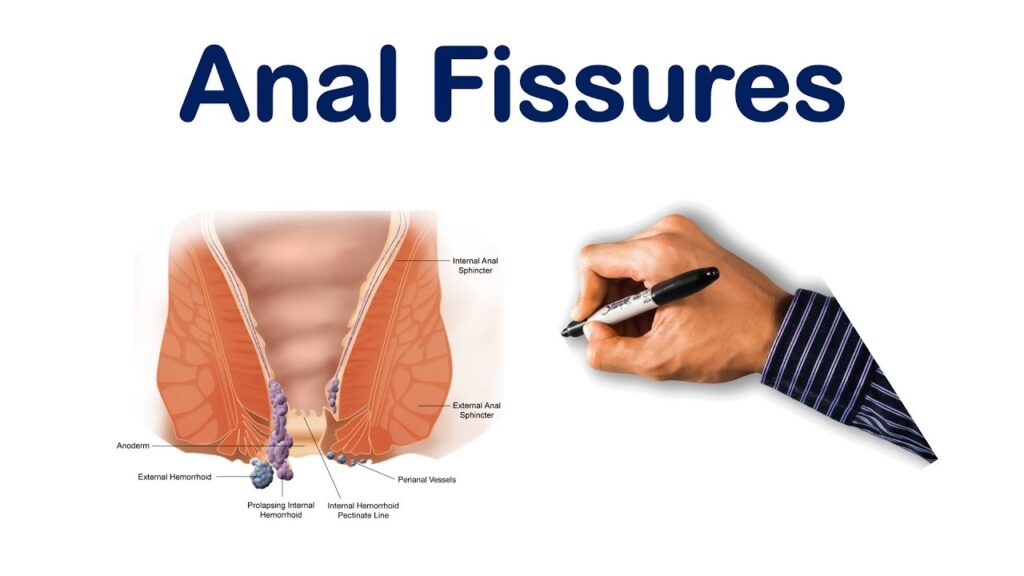
A small tear in the moist, thin tissue that lines the anus is called an anal fissure. The muscular opening at the end of the digestive tract where stools leave the body is called the anus. Constipation and straining or passing large or hard stools during a bowel movement are two common causes of an anal fissure. With bowel movements, anal fissures typically cause pain and bleeding. Spasms in the anal sphincter—a ring of muscle at the end of your anus—may also occur.
Anal fissures can occur at any age, but they are most common in young infants. The majority of anal fissures improve with simple treatments like eating more fiber or taking a warm water bath. Anal fissure patients may require medication or, in rare cases, surgery.
Fissure in ano, commonly referred to as an anal fissure, is a small tear or crack in the lining of the anal canal that can lead to significant discomfort and bleeding. This medical condition, while often distressing, is fairly common and affects individuals across a wide age range. The primary symptom associated with an anal fissure is pain during and after bowel movements, often accompanied by bright red bleeding. Understanding the causes, types, symptoms, diagnostic methods, treatment options, and preventative measures can greatly assist those affected in managing and overcoming this condition.
The most prevalent symptom of an anal fissure is a sharp pain during bowel movements, which can persist for several hours afterwards. Other notable symptoms include visible blood on the stool or toilet paper, a burning sensation or itchiness around the anus, and in some cases, a visible tear or crack near the anus. Chronic fissures might also present with a small external lump or tag near the anal verge, known as a sentinel pile, indicating underlying issues that require medical attention.
Anal fissures can be classified into two main types: acute and chronic. Acute fissures are those that have occurred recently and typically heal within a few days to weeks with proper care. Conversely, chronic fissures are characterized by their persistence for more than six weeks, often failing to heal without intervention due to underlying issues such as increased sphincter tone leading to decreased blood flow to the area.
The primary cause of an anal fissure is trauma to the anal canal, which can result from passing hard or large stools during a bowel movement. Other contributing factors include chronic diarrhea, anal sex, or childbirth. Conditions that affect the bowel and result in inflammation, such as inflammatory bowel disease (IBD), can also predispose individuals to developing fissures. In some cases, no clear cause is identified, which necessitates a thorough examination to rule out other potential conditions.
Diagnosis of an anal fissure is primarily clinical, based on the patient’s history and a physical examination. A visual inspection of the anus usually suffices, but if the diagnosis is uncertain, or if treatments fail to resolve the fissure, further examinations may be required. These can include an anoscopy, where a small tube is used to examine the inside of the anal canal, or a sigmoidoscopy to rule out other conditions like inflammatory bowel diseases.
Treatment for anal fissures typically begins with conservative measures aimed at softening the stool and reducing strain during bowel movements. High-fiber diets, increased fluid intake, and stool softeners are often effective first steps. Topical treatments such as nitroglycerin ointment or calcium channel blockers can aid in healing by increasing blood flow to the area and reducing sphincter pressure. For chronic fissures that do not respond to conservative treatments, surgical options like lateral internal sphincterotomy are considered to reduce sphincter pressure and facilitate healing.
Ayurvedic treatment focus on the root cause of disease. Focus is on aahar and vihaar that includes dietary recommendations and lifestyle adjustments. Alongwith this herbal medicines are given orally and for local application in anal fissures. It relives most of the patient, if in some cases symptoms still persist then kshar karma and kshar sutra para surgical procedure are done. Ayurvedic treatments is having very high success rate in treating anal fissures that is without any complications.
To prevent the occurrence or recurrence of an anal fissure, adopting lifestyle and dietary changes to ensure soft, regular bowel movements is essential. This includes consuming a diet rich in fiber, staying well-hydrated, practicing good toilet habits such as avoiding prolonged sitting on the toilet, and regular exercise to promote bowel regularity. For individuals with recurring issues, it may be beneficial to routinely use stool softeners or fiber supplements under the guidance of a healthcare provider.
In summary, while fissure in ano can be a painful and uncomfortable condition, understanding its symptoms, types, causes, and available treatments can empower affected individuals to seek the appropriate care. With a combination of medical treatment and preventive measures, most can find relief and avoid future occurrences of this distressing condition.
If your are looking for anal fissure treatment that is free from complications and side effects then you can reach us at Arogyam Piles Clinic and Research Center, located in Mohali, Chandigarh. Arogyam Piles Clinic is known for its Research based authentic ayurvedic treatment in anorectal diseases. To schedule an appointment with us you can visit our official website www.arogyampilesclinic.com or call +91 96467 64444
***We Promise, no spam!
The desire to live a long and healthy life and to attain the fulfilment of pleasure, wealth and fame is only possible by following ayurveda in life.
© 2024, All Rights Reserved.